It is perhaps understandable that the general focus for reproductive scientists working in ART might be on optimizing conditions for the oocyte and embryo.
After all, sperm will happily survive at a range of temperature and pH, including the 37°C and pH of 7.3 typical of fertilization media. It is clear, however, that the conditions during handling, preparation and storage can have a profound effect on the sperm, including the levels of DNA fragmentation1,2.
In his article regarding the optimization of sperm washing media, Mathew Tomlinson PhD discusses work done in his lab by Nadia de Rosa (in collaboration with CooperSurgical Fertility & Genomic Solutions) which highlights the impact of pH and bicarbonate on sperm motility.
In this project, a number of derivatives of a base medium were used to assess the impact of these two factors with the clear conclusion that high pH and high bicarbonate concentration gave the highest percent progression and sperm velocity, seemingly not at the expense of ‘burn out’ with sperm dying off sooner.
This approach is reflected in the ORIGIO Gradient Series. The key elements of these products (which include gradients and sperm washing medium) are, notably; alkaline pH, elevated levels of bicarbonate, antioxidants and (in the case of ORIGIO Sperm Wash) a higher concentration of human serum albumin.
Let us take a look at these.
As already highlighted, we have often handled sperm in a buffer or fertilization medium that has a pH of around 7.3 but the natural environment for sperm (seminal plasma and cervical mucus) is alkaline and higher pH positively influences a number of sperm functions including capacitation.
For example, intracellular calcium (via CatSper channels) and intracellular pH (pHi) are increased by raising the extracellular pH (pHo) which lead to significantly increased motility and hyperactivation (Achikanu et al, 2018).
This aspect of sperm biology underpins the design of the ORIGIO Gradient Series in which each product, whether gradient or sperm wash, has a pH of 8.0 to 8.5.
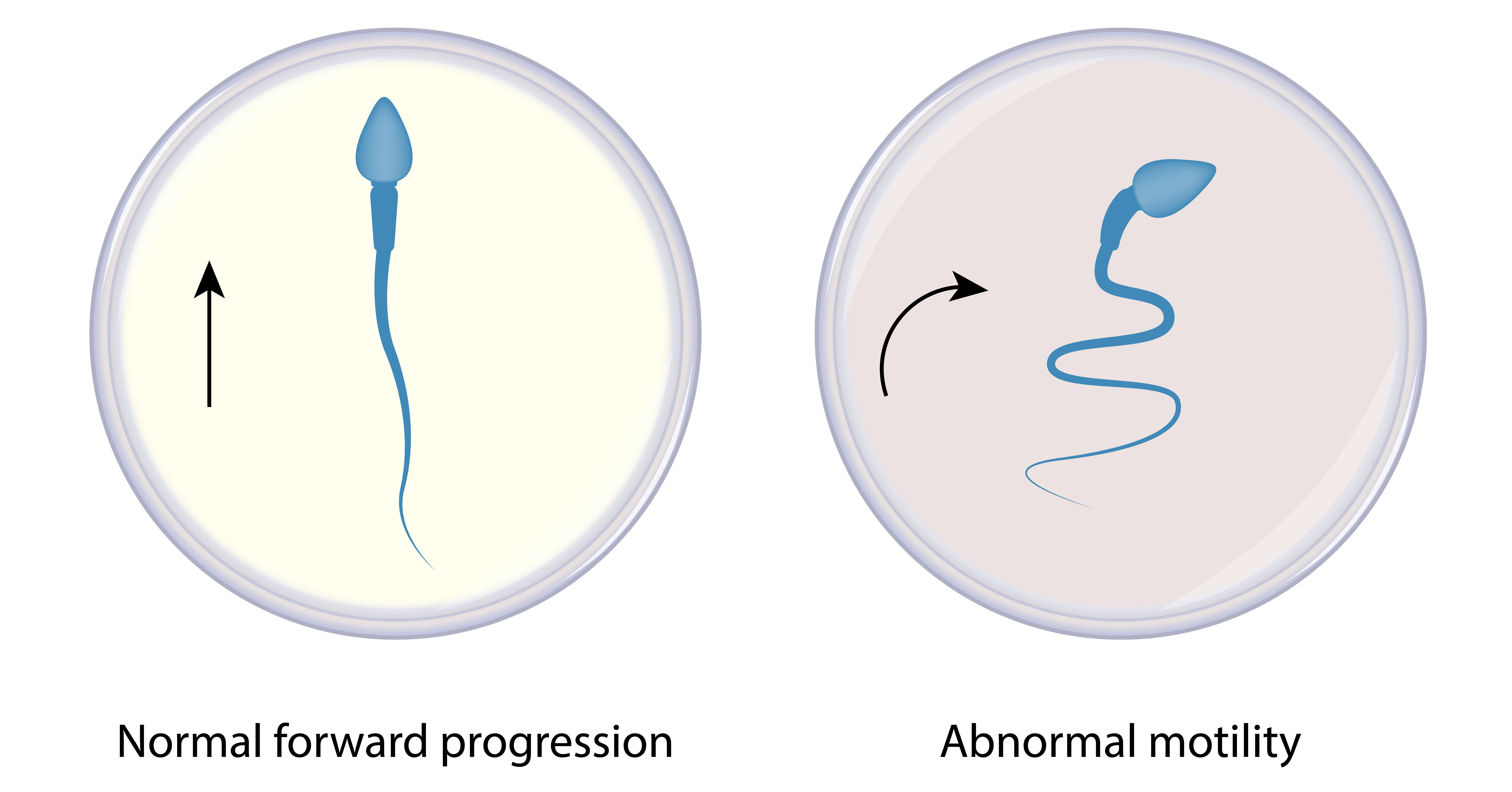
Similarly, an increased concentration of bicarbonate (HCO3–) is used in the ORIGIO andrology products but as an active component and not as a way of regulating pHo as for culture media. (The higher pH, as discussed above, is maintained using HEPES.)
HCO3– has long been associated with sperm functions. Sperm motility is suppressed during their transit through the epididymes, where HCO3– concentration is very low, with a rapid resumption upon mixing with fluid of the seminal vesicles at ejaculation.
Indeed, sperm with poor motility may be activated using media containing high levels of HCO3–.3 Other reports show a clear influence of HCO3– on capacitation, hyperactivation and acrosome reaction.4
The role of reactive oxygen species
The role of reactive oxygen species (ROS) in sperm function is well documented. At physiological levels, ROS perform a key role in sperm capacitation but higher levels of oxidative stress can lead to membrane damage via lipid peroxidation and, ultimately DNA damage.5
Sperm are more prone to oxidative stress after preparation so providing some protective measures is a prudent approach: the ORIGIO range contains several components with antioxidant effects, most notably taurine.6
Human serum albumin (HSA) has antioxidant properties7 but also supports sperm motility and protects against sperm DNA damage. It also is found in high concentrations in the female reproductive tract. ORIGIO Sperm Wash has double the usual concentration of HSA at 10 mg/ml to provide extra protection to the prepared sample.
Additional osmolality gradient
A final important development in the ORIGIO Gradient Series is that the system employs not only a density gradient but an osmolality gradient.
The elements of the gradient are formulated with osmolalities such that the sperm will transit from seminal fluid with high osmolality8 through the 40% layer (317-333 nOsm/kg) and 80% layer (297-313 mOsm/kg) before being washed in Sperm Wash (272-288 mOSm/kg) whose osmolality is more typical of sperm buffers and fertilization/culture media.
This approach limits the potential harm of osmotic shock during the density gradient centrifugation.
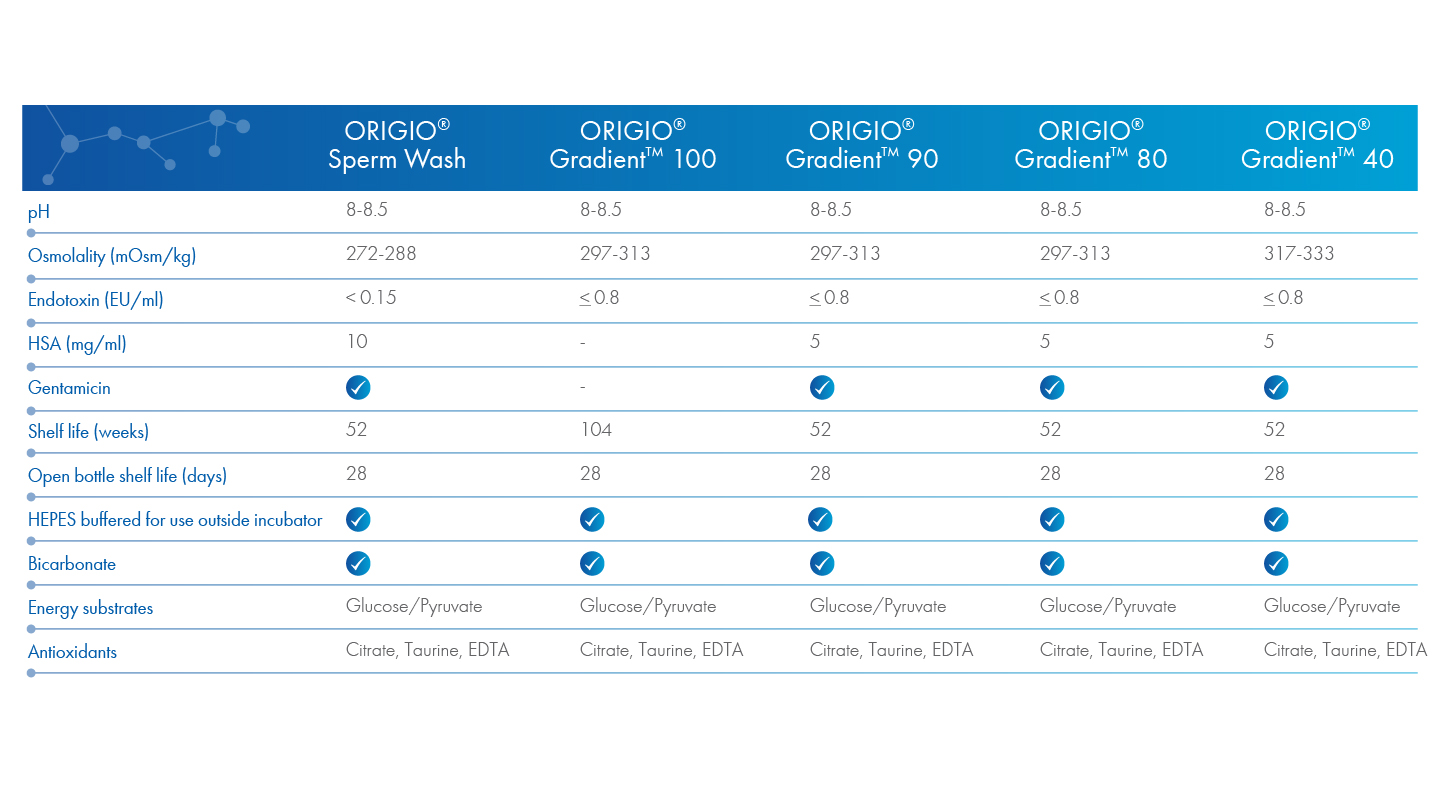
Using the ORIGIO Gradient Series and Sperm Wash, with the design elements described above, may help preserve sperm integrity and promote motility. All this would be for naught, however, if handling and preparation procedures employed by the laboratory are not optimized and well-controlled.
The general advice is to limit the time between sample production and preparation, ideally beginning as soon as the sample has liquefied. Where possible, it is also preferable to keep the time between preparation and use to a minimum though scheduling of procedures can make this tricky.
In all cases, however, the sample should be processed and kept before use at room temperature and not 37°C as the higher temperature may result in a faster rate of spontaneous DNA damage (especially in a CO2-enriched environment).1 It should be noted that the ORIGIO Series is designed to be used at room temperature.
View our Andrology Products
New research on Andrology has been published!
PICSI® Dish and SpermSlow™ Media
by Steve Fleming PhD – Director of Embryology, CooperSurgical

Summary
The ORIGIO Gradient Series aims to put the sperm first and provide the best environment to promote motility and sperm function whilst protecting against damage.
It is optimistic to expect significant increases in clinical outcomes such as clinical pregnancy rate but the system should deliver sperm in the best possible condition which may lead to marginal gains.
 David Morroll PhD
David Morroll PhD
David has worked as a Clinical Embryologist since 1986, training in Manchester, where he also completed his doctorate studies. He has since managed laboratories in a number of UK IVF units including those in Nottingham, London and Leeds. He has also consulted to IVF units in Malta, India, the Philippines and Zimbabwe.
He joined ORIGIO as Director of Embryology in November 2011 and, in January 2019, was appointed Director of Clinical Support for CooperSurgical Fertility and Genomic Solutions, focusing on post-marketing clinical studies, QA/complaints and laboratory audits.
He has previously served as Chair of the UK Association of Clinical Embryologists (ACE) and Association of Biomedical Andrologists (ABA), and was involved with several working groups, notably the HFEA Expert Group on Multiple Births after IVF. David has a keen interest in quality management, including ISO certification and External Quality Assurance.
Further Reading: Expert Article
Mathew Tomlinson PhD, Consultant Scientist in Andrology and Scientific Director at Procreative Diagnostics, has written an article Optimizing Theraputic Sperm Washing Medium: Why Are There Clear Differences in Progression and Sperm Velocity Between Products? in the first 2020 edition of our scientific newsletter – ART Scientific.
To read the article – click here
Our ART Scientific publication explores current topics of interest in our industry. It is written by a community of experts in the field and has a science focus at its heart.

 My Clinic is in the United States
My Clinic is in the United States My Clinic is in Canada
My Clinic is in Canada