
At CooperSurgical Fertility and Genomic Solutions, our aim is to help clinics deliver better outcomes for families, by improving success rates.
Scientific innovation plays an important role in helping us achieve this goal. In 2018, we launched our new PGTaism technology platform in the US and in the UK and Ireland at the start of this year. The first of its kind, it uses artificial intelligence (AI) and machine learning to improve preimplantation genetic testing ( PGT).
After clinics take a biopsy from embryos, the removed cells are tested to identify which embryos have the right number of chromosomes (46). Using AI and sophisticated mathematical algorithms, the system is able to make more robust and less subjective calls than a person undertaking analysis on their own.
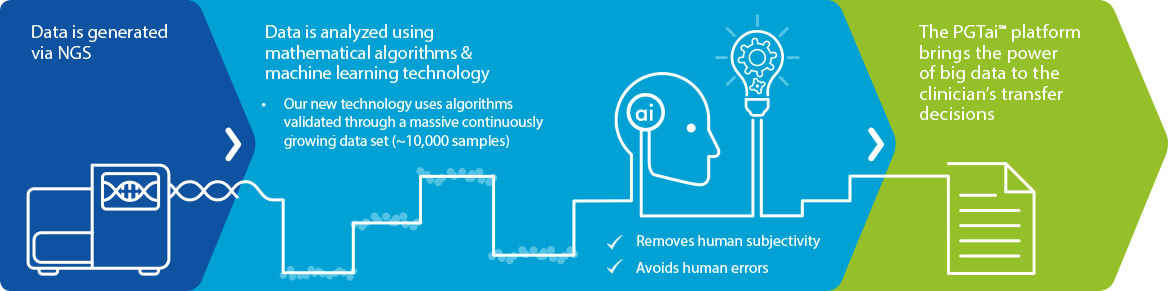
The technology also draws on test results of biopsy samples taken from embryos that resulted in a healthy life at birth, to better determine which embryos have the correct number of chromosomes. This is another unique feature of the platform. As more live-birth results are added and our database grows, our algorithm and reports will become even more robust.
Many women are delaying having children, but as maternal age increases, fertility decreases, particularly after the age of 35.1 One of the main reasons for IVF failure with advancing maternal age is that embryos from women over 35 are more likely to have the incorrect number of chromosomes.
Data suggests that if you select an embryo with the right number of chromosomes using PGT-A, the impact of maternal age on IVF outcomes may be reduced. For example, a 40-year-old using PGT-A can have comparable success to a 35-year-old, not using PGT-A, if this type of embryo is available in their IVF cycle. 2,3
This PGT technique can also help patients with a history of recurrent miscarriage as an embryo with the wrong number of chromosomes is far more likely to miscarry.
The potential for this technology to be used more widely is substantial and we are currently conducting tests covering tens of thousands of IVF cycles
a year.

Scientific innovation in other areas of IVF is also helping women get pregnant. IVF success rates increased rapidly following the birth of Louise Brown in 1978, but the rate of improvement has slowed over the past five to ten years.
The developments, additions and marginal gains we can make to IVF products, processes and procedures are therefore key.
Another area of focus for improving implantation rates and reducing miscarriage rates, often an issue for women of advanced age, involves using the human cytokine in culture media. This is the complex solution in which embryos develop for five to six days following fertilization prior to being transferred to the uterus.
Culture media containing granulocyte-macrophage colony-stimulating factor (GM-CSF) performs two roles. Firstly, it provides all the essential nutrients to support embryo development during this key period. Additionally, GM-CSF has been found to improve communication between the embryo and the endometrium, creating the right environment for a successful pregnancy.
3 days of embryo culture in GM-CSF containing medium improved live birth rate*
*Ziebe et al., A randomized clinical trial to evaluate the effect of granulocyte-macrophage colony-stimulating factor (GM-CSF) in embryo culture medium for in vitro fertilization. Fertil Steril. 2013 May;99(6):1600-9.
We are continually working with clinics to measure the success of using our GM-CSF enriched culture media. This is important because patients need transparent advice, with supporting evidence, about what treatments may help prevent repeat pregnancy loss or implantation failure.
A further innovation, introduced to safeguard the handling of gametes (sperm and eggs) and embryos, has been electronic witnessing.
Our RI Witness™ system was the first to introduce RFID (radio-frequency identification) technology to improve security in laboratories.
As well as helping prevent potential errors, such as male and female samples from different couples being paired, it operates as a powerful laboratory management system.
While laboratory staff members are handling samples during an IVF cycle, RI Witness continually gathers data provided by the RFID tags attached to the plasticware in which the samples sit.
It tracks how long procedures take, how long samples have been out of incubators, and which staff members have handled which samples. These are all processes that can and may affect the success of a pregnancy.
Using RI Witness, clinics have the advantage of identifying the processes used that led to positive results.
This is significant as large IVF laboratories may be managing as many as 50 cycles at the same time. Clinic groups can also share data, between clinics, to create standardized protocols that follow the processes yielding the best results.
It is encouraging when scientific innovations stand the test of time
In 1978, Harry Wallace designed the world’s first commercially available embryo transfer catheter that was used in the first successful IVF treatment. This led to the birth of Louise Brown.
To this day, we continue to manufacture the Wallace catheter that minimizes trauma, suits different patient anatomies and enables confident positioning in the uterus. It remains popular with gynecologists as it continues to achieve positive results.
As an established medical company, we are in a unique position to continue innovating. We can draw on the knowledge of scientists, experts, and pioneers who have worked in IVF over the past 40 years.
Alongside knowledge-sharing and providing top-quality IVF training, developing scientific innovations will always remain at the heart of what we do.
This article originally appeared in The Times Supplement ‘Understanding Fertility‘ published by Raconteur.

 My Clinic is in the United States
My Clinic is in the United States My Clinic is in Canada
My Clinic is in Canada
